There’s a lot to lose sleep over these days, so learning more about what keeps us up at night is important for health. We dove into the data and found that many people might have a sleep issue—and not even know it.
People have insomnia for a variety of reasons ranging from depression to medication and even perfectionism. But what is insomnia and why is it a big deal? Isn’t it just feeling tired and maybe a bit sluggish? Nope. As reported in the Journal of Clinical sleep medicine, insomnia is often “misreported, mishandled, and just plain missed” which is a problem because it’s actually a risk factor for a variety of mental and physical issues.
What is insomnia?
If we’re going to talk about insomnia, then we need a definition of what it is, so we referenced these standards from “Insomnia: Definition, Prevalence, Etiology, and Consequences”:
- difficulty falling asleep, staying asleep, or nonrestorative sleep
- this difficulty is present despite adequate opportunity and circumstance to sleep
- impairment in sleep is associated with daytime impairment or distress
- sleep difficulty occurs at least 3 times per week and has been a problem for at least 1 month
Number 2 is probably the most important distinction for people to understand as sleeping in an environment that doesn’t allow for rest does not mean you have insomnia but rather are a victim of circumstance or your own habits.
Finally, insomnia can either be acute or chronic. Acute insomnia is short lived and could be due to a traumatic event, work stress, etc, whereas chronic insomnia can last a minimum of several months and be caused by medication, long-lasting emotional upset, and more.
Data hints to hidden insomnia
Since there’s evidence that insomnia is often missed, we decided to survey our community. We asked 12,000 people questions about their sleep, medical history, and insomnia status.
Insomnia is reported to affect a third of adults globally, but only 22% of our respondents either self-described as having insomnia or officially were diagnosed as having it.
While that’s less than a third, it tracks with what our data showed: an extra 12% of people who didn’t identify as having insomnia showed evidence in their responses that they very well might have it.
But how could a third of adults have insomnia with such a large share unaware that they might be suffering from it? Insomnia is commonly missed by primary care physicians unless specifically asked for by patients, and with over 51% of our respondents reporting that they’ve been concerned about their sleep and 19% of those worried for more than five years, we figured it would be worth diving into the data to see how many people might be missing an insomnia diagnosis.
How we identified the hidden or unaware insomnia
Respondents answered 40 questions, and within those we were able to prompt information that could potentially point towards insomnia without having respondents needing to affirm a diagnosis. We used the criteria from the definition of insomnia above, with one slight modification as listed changing “sleep difficulty occurs at least 3 times per week,” to “daytime functions impeded at least 3 days during the week due to a lack of sleep,” since our survey did not list the specific criterion.
First, we asked if people had issues with sleep.

If a respondent said “yes” to any of these questions, we consolidated them into one group.
Then we found many people experience environmental disruptions like loud noise, light, etc. A quarter of people are blaming their partner or family for keeping them up.
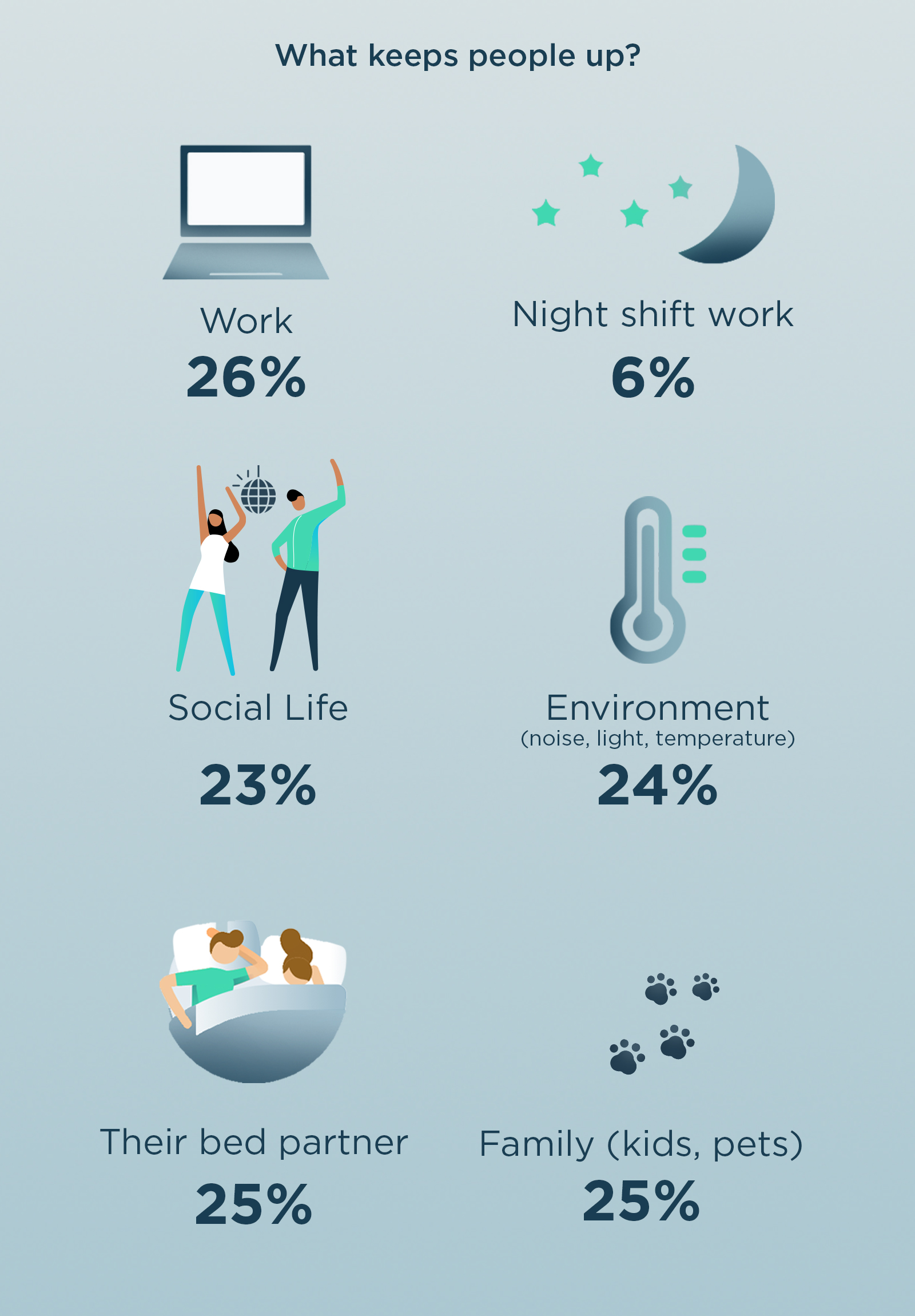
Then from this group, we eliminated these respondents from possible hidden insomnia, because insomnia means someone still has difficulty sleeping even when conditions are right.
After this, we made one more filter. We eliminated respondents who had less than 3 days of daytime function being impeded by lack of sleep.
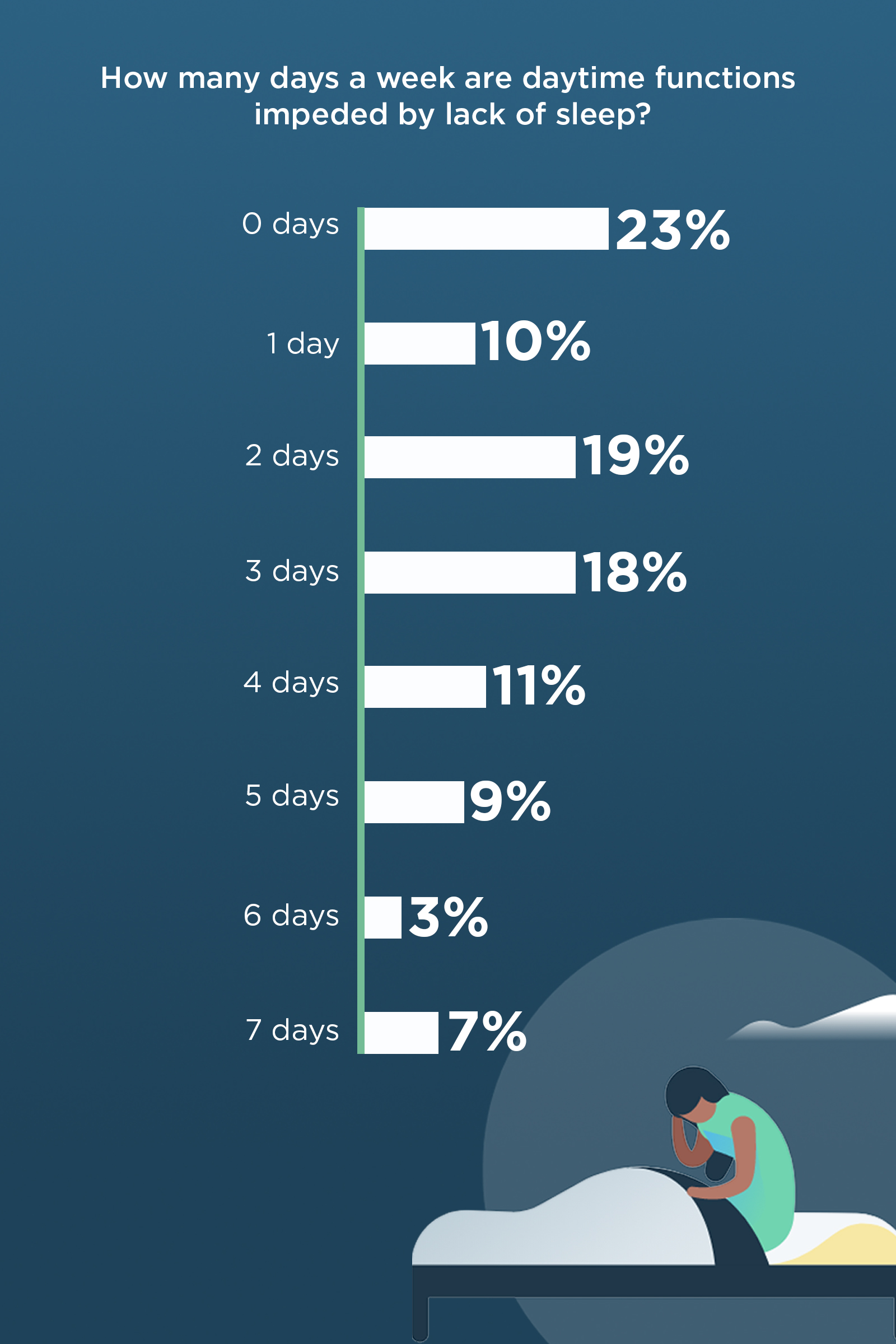
Based on the three criteria from above, we found that an extra 1,450 respondents, or additional 12.02% of total respondents, could have insomnia without knowing it. Add that amount to the combination of diagnosed and self-described insomnia of 22.22%, and we reach 34.24% which aligns with the literature above stating that up to a third of adults have insomnia and are many times not diagnosed with it.
And why is lacking a diagnosis of insomnia potentially a bad thing? When people who self-described as having insomnia were asked if they had been officially diagnosed with other diseases and conditions, they reported higher instances:

This means there could be a large swath of people not only missing an insomnia diagnosis but also potentially suffering from another condition without knowing or being treated.
Don’t sleep on it when it comes to your health
Sleep is an integral component of our health as sleep problems can impact quality of life and have real-world consequences ranging from poor performance and accidents to serious health issues. If you are diagnosed with insomnia, there are medicines that you can take and ways to harness cognitive behavioral therapy (CBTi) tactics for chronic insomnia that can help you focus on behavior and psychology to ease out of and reduce the condition.
If you are concerned about your sleep but don’t know where to start, then consider using a sleep diary. Doing so could help you recognize problematic patterns, but having this data readily available for your doctor could help get you on a faster and more targeted treatment plan. The Health Mate app, by the way, allows you to automatically edit a sleep log for Sleep and Sleep Analyzer users.
This study was conducted by Withings based on anonymous aggregated data from a global pool of 12,000 users who opted into our survey. Withings guarantees the confidentiality of personal data and protects the privacy of all its users. Therefore, all data used for this study was rigorously anonymized and aggregated in order to avoid any re-identification.